We often think of the nervous system as a single structure regulating our body. However, our nervous system has two very different parts, the sympathetic and the parasympathetic. In these stressful times, understanding how our bodies respond to stress, how stress affects our immunity, and the interaction between the two is vital for optimal health.
The human nervous system’s immediate response to stress is based on an animal-like instinct. However, we differ from animals because we have the capacity for meta-cognition — we are conscious and also aware of our consciousness. We have the capacity to reflect on things that we think and feel, which is an important component in managing our stress response.
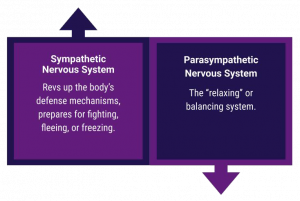
Our stress response is hard-wired into our nervous system, built into our DNA to enable our survival when we were being chased by a hungry lion. Today, that same hard-wired response is triggered when we are in major physical danger. When we experience stress of this kind, the sympathetic nervous system kicks into gear and does things like increasing our heart rate, dilating our pupils, causing our breath to quicken, and pumping oxygen to muscles that would be needed to flee to survive. To have the energy and resources for all of those important processes, the body shuts down other systems that are not considered critical during a major physical threat, such as digestion, reproduction, and immunity.
 Here’s where things get interesting… Nowadays, few people are faced with that intense kind of physical danger, but our stress response will still kick into gear when we have what’s called a “perceived” stressor, like a tight deadline at work, an argument with a loved one, or a fast moving pandemic that has uprooted our lives. Even if we aren’t being impacted directly, our mind can conjure up many different frightening scenarios as to how we (or people we love) might be impacted. Our sympathetic nervous system cannot tell the difference between an actual physical threat and an imagined or perceived threat and it will marshal all the same resources and turn on the same physiological systems even when we aren’t in actual physical danger.
Here’s where things get interesting… Nowadays, few people are faced with that intense kind of physical danger, but our stress response will still kick into gear when we have what’s called a “perceived” stressor, like a tight deadline at work, an argument with a loved one, or a fast moving pandemic that has uprooted our lives. Even if we aren’t being impacted directly, our mind can conjure up many different frightening scenarios as to how we (or people we love) might be impacted. Our sympathetic nervous system cannot tell the difference between an actual physical threat and an imagined or perceived threat and it will marshal all the same resources and turn on the same physiological systems even when we aren’t in actual physical danger.
The good news is that our parasympathetic nervous system counterbalances the response of the sympathetic nervous system by managing relaxation, rest, re-building, and the optimal functioning of our immune system. The even better news is that because of our capacity for meta-cognition, if we realize we are in a stress response and we are not in actual immediate physical danger, we can consciously choose to intervene in that process and switch over from a sympathetic response to a parasympathetic response. When our body is in the parasympathetic state, it directs energy towards supporting systems like digestion, reproduction, and immunity. When we take time to consciously relax, our bodies release muscle tension, lower blood pressure, slow the heart and breath rates, and reduce hormones like cortisol (aka – the “stress hormone”).
As a teacher of mind-body medicine for stress reduction and boosting health and well-being, in times like these, I don’t see relaxation or self-care as luxuries; I view them as crucial ways to support our immunity and our health.
How do you help your body switch over to the parasympathetic nervous system and support your immune system to be strong and fully functional? Meditation is an incredibly powerful tool for this. At IONS, we have conducted research on how meditation helps support people’s health in a variety of populations and health conditions, including reducing the stress response, cortisol, and glucose intolerance in pregnant women in our study Effects of a Mindfulness-Based Intervention on Distress, Weight Gain, and Glucose Control for Pregnant Low-Income Women. We recently completed research phases in two of our studies on the impact of meditation on depression and anxiety symptoms in older adults: iRest (Integrative Restoration) Meditation for Older Adults with Depression Symptoms and Internet Mindfulness Meditation Intervention (IMMI) Improves Depression Symptoms in Older Adults (for all of the papers published on these studies, see the Additional IONS Research section below). Our Director of Research, Dr. Helané Wahbeh has also published a systematic review on Mind-Body Medicine and Immune System Outcomes.
Dr. Wahbeh, who is also a naturopathic physician, is a very skilled meditation facilitator. Try out the short (8 minute) meditation that she recorded at a recent Noetic Global Gathering which specifically guides you into a meditative state that supports your immune system. Additionally, we just completed a free online ConnectIONS Live: Noetic Approaches to Health & Wellbeing webinar that featured experts in the field of noetics discussing ways to support your health and wellbeing, which also includes additional meditations.
Additional IONS Research
iRest (Integrative Restoration) Study
IMMI (Internet Mindfulness Meditation) Study

Nina Fry-Kizler, MA, is a Program Development Specialist & Science Liaison at IONS. A former professor in the Holistic Health Education Masters Program at JFK University, she teaches classes on the psychology and physiology of stress, the challenges of change/transformation, energy models of healing, wellness coaching and mind-body approaches to self-care. Nina was trained in the Mind-Body Medicine Professional Training program from the Center for Mind-Body Medicine and as a Birth Doula through Doulas of North America.
